Before Kurt Edwards was a nurse, he was a Teamster.
For 10 years he worked the graveyard shift driving a forklift at a distribution warehouse that supplied more than 100 A&P grocery stores across the greater Detroit area. “I figured the food market was never gonna fold,” he tells me. “But this was during the W. Bush years, and a lot of people were losing jobs. We came in one day and got pink slips.”
A&P was pulling out of the Michigan market due to bankruptcy. “I thought, What am I gonna do?”
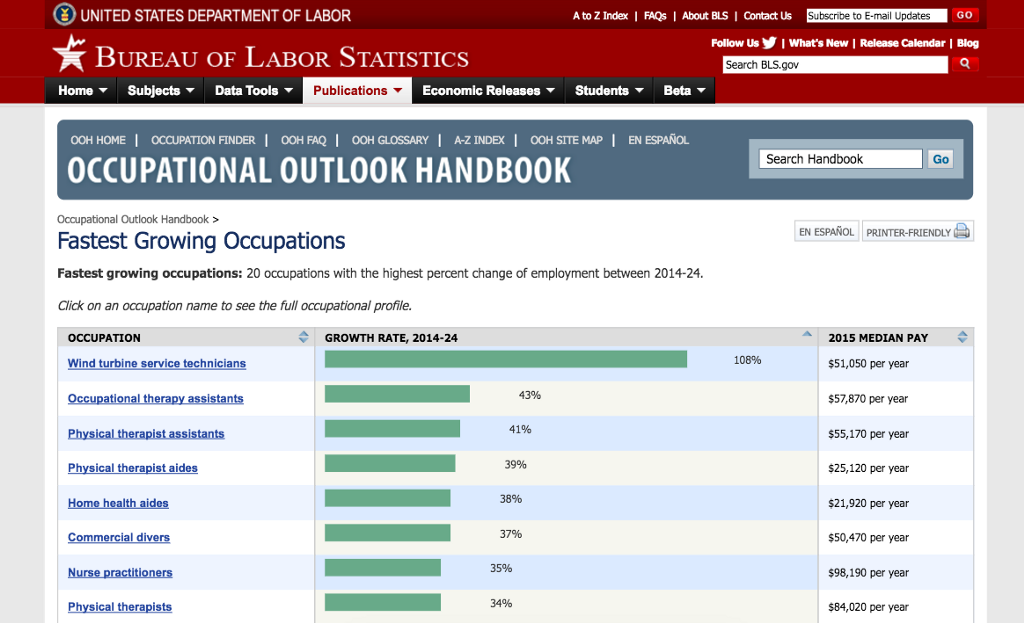
Some co-workers planned to find warehouse work elsewhere; others thought the logical next step was trucking. Edwards, on the other hand, considered a bigger leap — one that an increasing number of American workers are also considering these days. According to the Department of Labor, most of the fastest-declining occupations are in blue-collar industries while most of the fastest-growing occupations are in the feminized service sector — or so-called pink collar industries like nursing. For instance, employment of nurse practitioners is projected to grow by 35 percent from 2014 to 2024, much higher than the 7 percent projected average growth rate for all other occupations.
Edwards’ biggest stumbling block was the how of it all. The transition seemed impossible given that he was nearly 50 years old, with limited savings and no experience whatsoever in health care. His timing, though, was perfect: Detroit Mayor Kwame Kilpatrick had just instituted a program wherein if you passed the standardized nursing entrance exam you could attend nursing school for free.
“I’d never heard of male nurses,” Edwards remembers. “It was almost laughable. But I reasoned it was one career where I’d never have to worry about finding a job, since I’d read about nursing shortage predictions.”
Edwards passed the test and was accepted into nursing school, though acceptance from his instructors was harder to gain. One old school nurse even told him she believed men had neither the compassion nor the empathy for the job. “Initially, I was shocked. I was there to learn how to become a nurse, and she was telling me I didn’t have what it takes because I lacked these attributes. So I made up my mind to develop them.”
He was the only one of his five male classmates to graduate, in 2010, and was soon hired at the Sheffield Manor Nursing and Rehab Center, a two-story gray brick building in a ramshackle neighborhood on Detroit’s West Side. “I was offered $70,000 annually — $10,000 more than I was making at the warehouse,” he says.
He quickly found, however, it wasn’t going to be easy. At school he always had someone to guide and assist him, but without that help, he began doubting himself. “I was fearful,” he remembers. “I made the career change solely based on financial stability. So to come into a setting where people’s lives were on the line — where one mistake could actually kill them — was eye-opening. Plus, we’re heavily regulated by the state and certain errors can cost you your license.”

Edwards, a former paratrooper in the Army, says his empathy and compassion did in fact need improvement. “I had to learn not to always be the tough guy,” he admits. He did so by paying attention to how other nurses treated patients. “A gentleman sitting by the desk defecated on himself the second week I was on the job,” he says. “You could smell the bowel movement on the whole floor — it was horrible. I immediately stepped toward him and raised my voice, shouting, ‘Sir, go to your room right now! Get away from our desk! Go to your room!’ Another female nurse who knew this man stood up calmly and said, ‘Mr. So-and-So, will go to your room if I buy you a pop?’ She bought him a pop, brought it back and he went to his room with her. When I came to work the next day the man was dead; it turned out he had terminal cancer and was very sick. I vowed to never speak to a patient like that again.”

By 2022, the estimated total number of nursing vacancies is projected to be more than a million. That’s because, according to the latest figures from the Census Bureau, there are currently more than 76 million baby boomers. With the over-65 population set to triple by 2030, a report from the American Hospital Association has predicted the following:
- More than 60 percent of baby boomers (roughly 37 million people) will suffer from multiple chronic conditions.
- More than 25 percent (roughly 14 million people) will be living with diabetes.
- More than 33 percent (21 million people) will be obese.
- Nearly 50 percent (26 million people) will suffer from arthritis.
Shortages are expected to play out across the entire continuum of medical care, but nursing is predicted to take the largest hit. “We’re simply going to need more nurses of either gender,” notes sociologist Marci Cottingham, who adds that men have historically been an untapped resource in the field. The rationale for focusing on men, she explains, is that they could make unique contributions to medical staffs — like lifting patients more easily. The rhetoric and recruitment efforts just need to be polished to get them into the fold.
Eager to compensate for the impression that nursing is a woman’s job — the word nurse is synonymous with breast-feed — campaigns focused on recruiting more men into the profession have typically employed hyper-masculine imagery. In a 2013 study, for instance, Cottingham found that more than 20 percent of these recruitment materials (brochures, posters, videos, nursing web pages and newsletters) relied on portraying men in a very stereotypical manner: i.e., hyper-athletic dudes with bulging biceps. “You see a lot of strange imagery included in this type of recruitment,” she explains. “Nurses playing basketball, skiing and snowboarding — athleticism is featured to subtly reinforce that you can be a nurse and not have your masculinity challenged.”
Case in point: The Oregon Center for Nursing’s 2002 campaign “Are You Man Enough To Be A Nurse”:


The American Association of Male Nurses deployed similar macho themes in its current campaign to reach 20 percent male enrollment in nursing programs throughout the U.S. by the year 2020 (aptly named “20×20: Choose Nursing”). The poster features an OR nurse wearing a surgical mask next to an image of the same nurse wearing a mask for mountain climbing in extreme weather. “Risk-taking/adventure, athleticism/physicality and detachment from emotion are reflected in the image,” notes Cottingham.

“Of course, when we’ve promoted the idea that nursing can be done by men who have athletic and outdoor interests, some women have criticized us for projecting that as an image for nurses,” Ed Halloran, AAMN’s chairman of the board, tells me. “But I think it’s completely natural for people who were brought up doing these activities to promote that they still do them while also being a nurse.”
Cottingham says what surprised her most in her study was the extent to which so little of what’s portrayed in the recruitment videos jives with reality. “It’s kind of a caricature,” she says. “I’ve done other research with nurses and have a good sense of what their day-to-day life is like and the many raw emotions they have to deal with. A lot of that’s ignored in these recruitment efforts.”
“I think this is false advertising,” Edwards says of the “Men in Travel Nursing” video above. “They need to market nursing for what it really requires: Patience, compassion and empathy — all those things my old nursing school instructor claimed women had naturally and men allegedly lacked. That’s nonsense. Of course men have these qualities — we’re just taught from a young age not to use them.”

The combative reception Edwards received from his older female instructors in nursing school has historically been the case, says Halloran, a registered nurse since 1964. “Traditionally, the biggest challenges of getting men to join the nursing profession is that women don’t want them there. I sadly concluded it was difficult for men to finish educational programs — or even to be admitted to them — because many of the values they had were anathema to those women had in the field. Namely, that [to women] it was a calling instead of a job.”
In 1980, Halloran was invited to speak at the National Male Nurses Association, which was founded in the 1970s with the goal of acknowledging and supporting men in nursing. The first NMNA meeting he attended at Rush University in Chicago was sparsely attended — so much so that by the end of it, he’d been elected president of the organization, which has since changed its name to the aforementioned American Assembly for Men in Nursing.
In 2012, he joined the admission committee for the nursing school at the University of North Carolina, where he teaches , and where his efforts to recruit male nurses have been known to ruffle feathers. One particular case of feather-ruffling stands out to him: A number of male applicants wanted to be nurse anesthetists, he remembers, which meant they would first become nurses and then attend the School of Anaesthesia. “I said it was important for us to have men in the school — even if they just wanted to go on to become nurse anesthetists and make upwards of $150,000 a year. ‘What’s wrong with nurses aspiring to make that kind of salary?’ I argued. It always struck me as odd that you were expected not to ask for too much pay.”
Halloran, however, says any discussion about salary in the nursing realm was seen as a faux pas. This was a calling, after all — not a job. “I received tremendous blowback from my fellow teachers for wanting to admit men who had inclinations of being anything other than a staff nurse in a hospital and follow the usual career path. The school determined these weren’t ‘suitable applicants’ because they were just there as a stepping stone to something else.”
Nursing’s feminine roots can be traced back 150 years, when the profession began to organize around principles espoused by Florence Nightingale. While Nightingale’s emphasis on proper hygiene, careful data collection and rigorous standards for performance transformed nursing from low-status work to a respectable career option for unmarried women, men were excluded from her training programs. As nursing historian Tom O’Connor notes, “This feminization stemmed from Nightingale’s belief that men weren’t suited to nursing. She wrote that men’s ‘hard and horny’ hands weren’t designed ‘to touch, bathe and dress wounded limbs, however gentle their hearts may be.’ She believed a good nurse should be ‘nurturing, domestic, humble and self-sacrificing.’”

As nursing evolved into a stereotypical female role, men became almost fully excluded. “Because of that,” explains Cottingham, “the profession developed in opposition to being a physician and the feminine traits of being compassionate, nurturing and emotionally empathetic were emphasized.”
By 1930, there were more men employed as piano and organ tuners than as trained nurses. A half a century later, many nursing schools continued to bar male students. In fact, it wasn’t until 1982 when the Supreme Court ended the practice of barring men from a nursing education in a narrow 5–4 vote on the landmark case Mississippi University for Women v. Hogan. In the majority opinion, newly appointed Justice Sandra Day O’Connor wrote, “Rather than compensate for discriminatory barriers faced by women, the university’s policy of excluding males from admission to the School of Nursing tends to perpetuate the stereotyped view of nursing as an exclusively woman’s job.” Moreover, she believed, by ensuring that more women than men were able to find places in nursing schools, the school’s policy “made the assumption that nursing is a field for women a self-fulfilling prophecy.”

There are, of course, a critical mass of people in the U.S. who have been educated by nurses and are proficient using manuals developed by nurses: Medics from the Armed Services. “There’s tens of thousands of them in the United States,” Halloran points out. “It would make great sense for those medics to be recruited into nursing programs. As a matter of fact, I’m working on a project right now to make medics eligible to take state nursing examinations while they’re still on active duty.”
Cottingham suggests that economics could demand that men trade in blue collars for pink ones before long as well. “With the 2008 recession, we did see more men moving into these traditionally female service sector jobs out of necessity,” she notes. “Not at the rate we would certainly want, but there is precedent to suggest that if the economics change and these become high-paying jobs that men will move into them. So over time, these recruitment methods may become obsolete because the pay will ultimately be the decider.”
Edwards, at least, is sold on the profession: He recently entered his seventh year as a nurse despite not seeing an increase in other men entering the field. “There are very few male nurses where I work,” he says. “No matter what floor in the hospital I go to, let’s say there are 20 nurses, only one or two of them will be males — if that.”
And while he knows firsthand that a lot of blue-collar jobs are going away, he’s still pessimistic about an influx of men donning scrubs. “They still view it as a female-dominated field and consider it women’s work.”
It’s a shame, he says: He thinks there’s a real need for men in nursing. Not just to lift patients — but to lift their spirits, too. “Male patients can’t go home. It’s lonely. They’re sick. A lot of them aren’t getting visits from family members and need someone to talk to. The female nurses can’t really identify with them. So if the football game is on, I’ll take a minute to ask who he likes and why. We may debate the coaching strategy. That companionship is important — especially for older male patients — which is why gender diversity in nursing is desperately needed.”
“I would compare it to female truck drivers,” he continues, “who probably feel similar stigmas as male nurses. Some say only a certain type of person could do these professions. Nonsense. There’s no ‘certain type’ in nursing. We’re all doing the same thing: Helping other humans get healthy.”

